Clinical Problem Solving (MT5)
Clinical Problem Solving
The Clinical Problem Solving course is the fundamental course in differential diagnosis for the physical therapist in an orthopedic manual therapy practice. Participants learn a critical thinking model that systematically takes them through a process of analyzing evaluation data for a more specific tissue diagnosis, as well as a functional list of impairments. The specificity of the pathoanatomical model of differential diagnosis is combined with the more generalized approach of classification, providing a more specific treatment approach. Learn the value of the pathoanatomical model for more specificity in diagnosis and treatment approaches. Anyone can learn to manipulate, but learn when not to when to, why to, and how much. Ola Grimsby and Rick Hobusch developed this review course as a way to aid the students in their ability to grasp the principles and concepts of manual therapy for use in clinical problem-solving so that they could apply them to patient care and be able to pass their final examinations. This course is a cognitive/theory review course and not a practical technique course, but a technique review course will usually be scheduled prior to the practical technique testing. There is time between case reviews during this course to review treatment concepts, with labs to help with any cognitive misunderstanding of what the examiners may be looking for during the oral part of your practical examination.
The course is provided to Orthopedic Residency students as a review the week of their Final Practical Exam. Prior to the development of this course, 40% of students failed their examinations. For those taking this course, the fail rate was reduced to below 10%. This course is also of value to students from other schools of thought for a view of our multifactorial approach to diagnosis and treatment.
This course is open to credentials of PT, MD, DO
Course Dates and Cities:
MT5 Clinical Problem Solving (Seattle, Washington) February 06-08, 2025
MT5 Objectives
At the conclusion of the course the participant will be able to:
• Understand the difference between Systems 1 and Systems 2 Thinking.
• Understand and be able to apply a problem solving plan to a clinical problem for advancing clinical reasoning
• Perform hypothesis generation utilizing systems thinking, other joints or regions that may affect or refer to this area, and specific tissues of the joint or region involved.
• Understand and describe the multifactorial approach for differential diagnosis used by the OGL
• Understand how clinical reasoning is currently described in the physical therapy research.
• Describe the three clinical reasoning processes used for diagnosis from the empirico-analytical research paradigm.
• Describe a model of management reasoning that is also helpful in diagnostic reasoning from the interpretive research paradigm.
• Recognize the elements of patient/client management that require clinical reasoning and decisions to achieve optimal outcomes, with emphasis on the purpose of examination.
• Select a clinical reasoning strategy for the different foci of clinical reasoning and actions.
• Utilize a patient centered model of clinical reasoning.
• Recognize that reflection is a powerful tool in developing clinical reasoning through gaining experience “in action” and “on action,” to have “reflection for action.”
• Discuss the core dimensions of expert practice and the attributes of a master (expert) clinician.
• Understand how clinical reasoning relates to evidence· based practice, and how research evidence is only one of the forms of knowledge used in clinical reasoning.
• Recognize common clinical reasoning errors.
• Discuss implications for clinical reasoning when applying the International Classification of Functioning, Disability, and Health (ICF) within a larger Biopsychosocial model of health care as it relates to the rehabilitation problem solving form.
• Demonstrate knowledge of specific tissue differential diagnosis and how this will direct the manual therapy intervention.
• Recognize the pattern of a single· tissue lesion that may be underlying a multi·tissue lesion.
• Understand the general principles of examination and how they apply to evaluation and diagnosis of the patient.
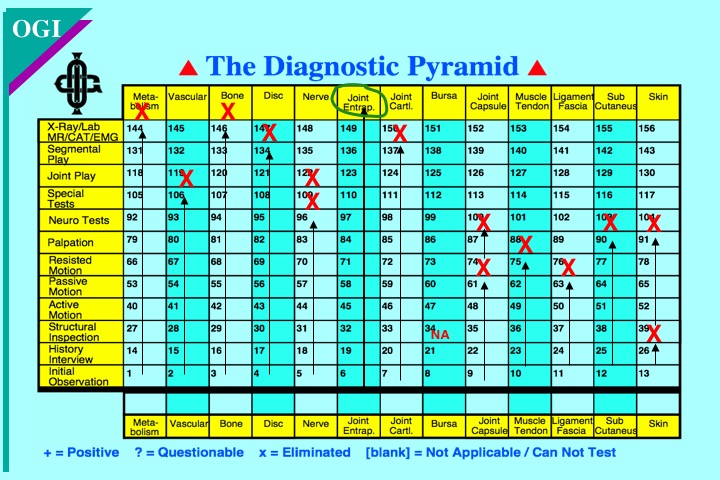
• Understand the purpose of the diagnostic pyramid and how to use the symbols.
• Utilize the diagnostic pyramid and perform a case presentation.

